What are allergies?
Allergies occur when your body’s immune system overreacts to substances that either enter or come into contact with your body. The word allergy covers many topics, but when people are complaining about “allergies” they are probably talking about environmental allergies. Environmental allergies include substances like dust, dander and pollen. These substances cause irritation of the nose and eyes and create symptoms like post-nasal drip, nasal congestion, itchy or watery eyes, sneezing, wheezing, and coughing.
How do I know if I have allergies?
You may already suspect that you have allergies, but your doctor will need to ask questions about your symptoms and your exposures in order to help determine if you are truly allergic. Some people suffer from seasonal allergies and notice that they have a runny or stuffy nose at certain times of the year or after they have been exposed to a cat or dog. Other people may have year-around symptoms without any seasonal variation and many patients will have both types of allergy. After your physician discusses your symptoms and exposures they will usually perform an allergy test.
How is allergy testing done?
Allergy testing is usually done in one of two ways. Typically, your physician will order a “skin-prick” test that checks your body’s reactions to multiple allergic materials such as different pollens, cat dander, dust, etc. The test is well-tolerated by patients and takes about 45 minutes to do in the office. Alternatively, your physician may order a blood test. You doctor will help determine which type of test is best for you.
I was tested for allergies when I was a kid and told I wasn’t allergic.
Just because you may have been tested and shown not to have any allergies as a child doesn’t mean that you can’t develop allergies as an adult. Many patients develop allergies later in life.
What are food allergies?
Food allergies occur when your body reacts to any food such as peanuts, shellfish, milk or eggs. You may experience symptoms such as tingling or itching of the mouth, hives, nausea, wheezing, or even more severe reactions such as anaphylaxis.
There is also a condition called “Oral Allergy Syndrome” where patients with pollen allergies also have reactions to specific related foods. For example, someone with a ragweed allergy may have a reaction to bananas or melons. Symptoms are usually limited to an itchy mouth or throat but they could be more serious.
What do allergies have to do with asthma?
Both allergy and asthma are the result of your body’s overreaction to exposures in the environment. A typical allergy patient reacts by experiencing nasal and/or eye symptoms. An asthma patient reacts with wheezing, cough or difficulty breathing. Many patients will have both conditions to a greater or lesser degree. It is estimated that 70-90% of patients with asthma have nasal allergies and 40-50% of patients with nasal allergies have asthma. Uncontrolled allergies may worsen asthma symptoms. In fact, many asthma patients find that their breathing problems are better controlled when their allergy symptoms are treated. We treat both allergy and asthma together at our practice.
What treatments are available for allergies?
There are three main treatments for allergies. The first treatment is avoidance, and as you would expect, it means trying to keep away from the substances that produce an allergic reaction. Avoidance measures include removing carpets and upholstery (to eliminate dust mites), keeping your windows shut in the warm months, using air filters, and protective covers. The second type of treatment includes the use of special medications such as nasal sprays, oral antihistamines and other medications. The third line of treatment is immunotherapy. Immunotherapy (also known as “allergy shots”) is a technique where your doctor uses small doses of allergic material to help your body learn not to overreact. At our office we offer the traditional allergy shots as well as a newer technique called allergy drops. Allergy drops have the advantage of allowing you to administer the therapy yourself at home without the need for any injection.
Can allergies cause sinus and ear infections?
Allergies have the potential to lead to many other issues including sinus and ear problems. Your sinuses are connected to your nasal passage through very small openings. Allergies cause these openings to swell, leading to a build up of mucus and infection within the sinuses. Similarly, allergies can cause swelling and blockage of the eustachian tube that connects the nasal passage to the part of the ear. Blockage of this tube can lead to a feeling of pressure in the ear, a build up of fluid, or a middle ear infection.
What can I do if I suspect I have allergies?
The best course of action is to meet with one of our physicians or our physician assistant to have a detailed discussion about your symptoms followed by a thorough examination with possible allergy testing.
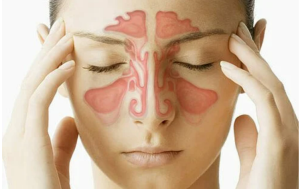 Sinuses are air-filled cavities inside our skull that help circulate and humidify the air that we breathe and shape our skulls. They have outflow tracts that drain into our nose which can sometimes get blocked or inflamed. When this happens, it can lead to a sinus infection. Acute Sinusitis, aka acute rhinosinusitis, is inflammation of the nasal cavity and surrounding sinuses. This can be caused by both bacterial or viral infections.
Sinuses are air-filled cavities inside our skull that help circulate and humidify the air that we breathe and shape our skulls. They have outflow tracts that drain into our nose which can sometimes get blocked or inflamed. When this happens, it can lead to a sinus infection. Acute Sinusitis, aka acute rhinosinusitis, is inflammation of the nasal cavity and surrounding sinuses. This can be caused by both bacterial or viral infections.