- Nasal Endoscopy: After topical anesthetic and decongestant agents are sprayed in the nostrils, a small, fiberoptic camera is placed into your nose to better evaluate the anatomy of your nasal airway and decide if VivAer is right for you.
- Cottle Maneuver: This is a test to evaluate for nasal valve obstruction. Place two fingertips on each side of your nose and gently press and pull outward. A positive cottle sign is noted if there is improvement in your breathing when performed.
- NOSE Score: This is a brief questionnaire we have you fill out in the office to assess the severity of your nasal obstruction. It is performed at your consultation appointment as well as post procedure for comparison.
Managing Your Allergies
- Nasal Saline Rinses: Also known as a Neti Pot. These are a fantastic way to irrigate your nasal cavity and sinuses to help remove unwanted mucous and allergens from the nose.
- Topical Nasal Steroids: Flonase (Fluticasone) is a commonly known topical nasal steroid spray that helps decrease nasal congestion, postnasal drip, and nasal obstruction. There are other types, both over the counter and prescription, that can improve your allergic symptoms as well. Please speak with your healthcare specialist to find out which would work best for you and your specific symptoms.
- Oral Antihistamines: These typically come in either 12 or 24 hour form and are taken once or twice daily to help combat allergy symptoms. Speak with your healthcare specialist to decide which antihistamine is best for you!
- Non-Medical Treatments: It is very important to be proactive this summer season when planning outdoor activities. You may benefit from wearing a mask if you know you will be outside for a long interval of time. To help combat allergies inside your home, we highly recommend air-purifiers, dust mite covers, and routine cleaning/dusting.
Is Acid Reflux Causing My Symptoms?
The stomach naturally produces acid to digest food. Sometimes this acid can make its way up the esophagus and into the throat, a condition called Laryngopharyngeal Reflux (LPR). LPR often occurs without heartburn, making it difficult to diagnose, and is often considered a “silent” disease.
What are some symptoms of LPR?
- Hoarseness, especially in the morning
- Chronic throat clearing or persistent cough
- Chronic sore throat
- A feeling of something caught in the throat (also known as globus)
- Excessive mucus/post-nasal drip
- Difficulty swallowing
- Restless sleep
How do we diagnose LPR at Montgomery County ENT Institute?
In order to properly evaluate your symptoms, we will use a camera to directly visualize your nose and throat (nasolaryngoscopy). This can be done in the office at the time of your visit with some topical anesthesia. This allows us to assess the cause of your symptoms. Signs of LPR in the larynx usually involve inflammation or redness around the larynx.
What is the treatment for LPR?
Typically treatment for LPR involves dietary changes and an over-the-counter Anti-Reflux medication. Here is a list of some foods to limit when suffering from LPR:
- Cigarettes
- Coffee
- Alcohol
- Peppermint, spearmint
- Tomatoes and tomato sauces
- Spicy foods
- Milk and milk products
- Orange juice
- Fatty foods
In addition to eliminating these foods, here are some additional tips to manage LPR:
- Eating smaller, more frequent meals
- Sleeping with your head elevated 4-6 inches
- Using a wedge pillow
- Placing a brick or block under the head of your bed frame
- Weight loss
Aren’t GERD and LPR the same thing?
Although GERD and LPR are related to acid produced from your stomach, they can be caused by different amounts and types of reflux. It’s possible to have GERD without LPR and to have LPR without GERD. Because of this, it’s important for an ENT professional to examine you.
What if my symptoms don’t go away?
Depending on the severity of symptoms and the in office exam, some patients require longer treatments than others. If symptoms are not improving, you might require an evaluation by another specialist (like a gastroenterologist).
How can Montgomery County ENT Institute help?
If you or anyone you may know is experiencing symptoms that might be from acid reflux or “silent” reflux, contact our office today for a thorough evaluation of your throat.
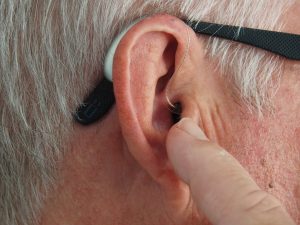
OTC Hearing Aid Q & A
Common Causes of Vertigo
- Benign Paroxysmal Positional Vertigo (also known as BPPV): This occurs when small crystals in the inner ear are displaced. Symptoms are brought about by positional movements – turning quickly, rolling over in bed, or bending over.
- Meniere’s Disease: This fluid imbalance in the inner ear may also cause vertigo. Vertigo episodes may also be associated with hearing loss, ear fullness, and tinnitus (hearing a noise in your ear). Symptoms may fluctuate.
- Deep Wax Buildup: Sometimes if there is a wax (cerumen) buildup up against the eardrum, some people can have problems with their balance as well as ear discomfort.
- Other ear related causes of vertigo: ear infections, labyrinthitis, vestibular migraines.
- Other non ear related causes of vertigo: low blood pressure, medications, head injury, stroke, tumor, or others.
6 Signs of a Sinus Infection
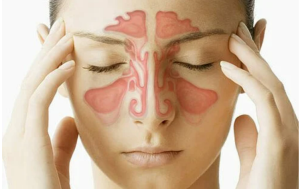 Sinuses are air-filled cavities inside our skull that help circulate and humidify the air that we breathe and shape our skulls. They have outflow tracts that drain into our nose which can sometimes get blocked or inflamed. When this happens, it can lead to a sinus infection. Acute Sinusitis, aka acute rhinosinusitis, is inflammation of the nasal cavity and surrounding sinuses. This can be caused by both bacterial or viral infections.
Sinuses are air-filled cavities inside our skull that help circulate and humidify the air that we breathe and shape our skulls. They have outflow tracts that drain into our nose which can sometimes get blocked or inflamed. When this happens, it can lead to a sinus infection. Acute Sinusitis, aka acute rhinosinusitis, is inflammation of the nasal cavity and surrounding sinuses. This can be caused by both bacterial or viral infections.- Thick, discolored nasal discharge: The color can vary, but may be yellow, green, or white.
- Facial pressure: Your face may be tender or painful (over your cheeks, in between your eyes, or even sometimes down to your teeth!).
- Nasal congestion: It might be difficult to breath through your nose from the increased mucous production in your nose.
- Loss of smell: Anything that blocks your nasal passage can take away your sense of smell. This can, in turn, affect your sense of taste as well.
- Postnasal drip: With the increased mucous production, it may be dripping down the back of your throat.
- Persistent symptoms for >2 weeks. Common colds or flus typically last 7-14 days. Anything persisting longer and not improving may be a sign of a bacterial sinus infection.
How to Fight Spring Allergies
March 20th is the official first day of spring! As we are excited for warmer weather and flowers blooming, some people are bracing themselves for a flare of allergies. Spring allergies can last anywhere from early March to beginning of June. When plants grow and bloom, they also produce pollen. Pollen from trees, weeds, and grasses can circulate in air and spread around with the wind or a breeze. Inhaling these can trigger a response in our body such as runny nose, postnasal drip, itchy eyes. If you suffer from Spring Allergies, here are are some helpful tips to help fight them this spring!
- Start taking your allergy medications before the spring allergy season begins (nose sprays or antihistamines)! This will help prevent manage symptoms by reducing your reaction before it starts.
- Remove allergen sources from your home the best you can. Keep your home and car windows closed. Use air purifiers to help circulate the air. Use central air conditioning.
- Use saline nasal rinses after a day of being outside (we love the NeilMed saline rinses).
- Change and wash your clothes after being outdoors.
- If doing yardwork outside, wear a mask and gloves to minimize direct exposure to possible allergens.
- Avoid peak pollen times, usually around 5-10 a.m. and at dusk. Pollen is also higher on warm, breezy days.
- Clean your pets with a towel when they come inside to reduce the spread of pollen.
What are some of the symptoms of allergies? Symptoms may vary from person to person, but can include some of the following: sneezing, stuffy nose, runny nose, itchy/water eyes.
How do I know if I have allergies? If you experience some of the symptoms of allergies listed above, it’s possible that you suffer from allergies. Formal diagnosis by an experienced healthcare professional is needed to confirm that you have allergies.
How can Montgomery County ENT help with your allergies? Here at Montgomery County ENT Institute, we discuss your symptoms and complete a thorough physical exam. We offer in-office formal skin allergy testing. This allows you to understand what allergies you have and at what time of the year they are likely to bother you. From there, we come up with a plan to treat your allergies and symptoms. This may include over the counter medications, nose sprays, or immunotherapy.
Signs you need a Hearing Test this Year!
 Hearing loss is the 3rd most common health problem in the United States. It currently affects 36 million Americans per day. There can be several reasons for hearing loss such as illness, certain medications, infection, trauma, allergies, or part of the aging process. It can also affect people of all ages. If you’re experiencing any of the signs listed below, it’s important to be further evaluated to prevent any further hearing loss and be cared for.
Hearing loss is the 3rd most common health problem in the United States. It currently affects 36 million Americans per day. There can be several reasons for hearing loss such as illness, certain medications, infection, trauma, allergies, or part of the aging process. It can also affect people of all ages. If you’re experiencing any of the signs listed below, it’s important to be further evaluated to prevent any further hearing loss and be cared for.
- Sudden change in hearing. It’s important to get tested as soon as possible in this situation.
- Difficulty differentiating noises. You struggle to hear other people talk in noisy environments such as restaurants or group events.
- You feel like everyone else is mumbling. You only catch parts of words sometimes.
- You often ask others to repeat themselves.
- Ringing or buzzing in the ears (tinnitus). This can be in both ears or just one. It can come and go or always be there too.
- You find it hard to understand conversations over the phone or when someone isn’t facing you directly.
- You’ve been turning up the TV volume too much.
- Missing out on day-to-day sounds, such as cell phone ringing or the birds tweeting outside.
- If you experience Vertigo.
What’s the difference between Hearing Screening and a Hearing Test?
Hearing screenings are commonly confused with a formal hearing test, also called Audiograms. Hearing screenings are quick, basic tests that one either passes or fails. The patient wears headphones and signals when noises are heard. Audiograms, on the other hand, are completed by Audiologists. They use a variety of different tests to determine your ability to hear sound. The patient sits in an enclosed sound-proof booth to complete the test. Audiograms are painless and take about 10-15 minutes.
How often do I need my hearing tested?
This answer varies from person to person. Typically, we recommend baseline Audiograms starting at age 65 years old. Depending on the results, one may require testing annually or every other year to monitor progress or any changes. If there is any sign of infection, fluid in your ear, sudden change in hearing, an Audiogram is also indicated as soon as possible.
How can we help?
At Montgomery County Ent Institute, we offer formal Audiograms with specially trained and highly experienced Audiologists. The test takes 10-15 minutes and are reviewed afterwards with Dr. Melissa Schwartz or one of our Physician Assistants. In addition to reviewing Audiograms, we also thoroughly examine the outside and inside of your ears, nose, and throat for any other underlying causes.
Call Today to Schedule an Appointment.
5 Ways to Prevent Nosebleeds this Winter
 Fall is officially over and winter is here! With this change comes cold weather, chilly winds, and less humid air which means it’s the season of nosebleeds. Nosebleeds, also known as epistaxis, are most commonly caused by dry air. Nosebleeds occur when the blood vessels that line the inside of your nose break and bleed. Therefore, it’s important to keep the inside of your nose moist. Here are 5 helpful tips to prevent nosebleeds during this holiday season!
Fall is officially over and winter is here! With this change comes cold weather, chilly winds, and less humid air which means it’s the season of nosebleeds. Nosebleeds, also known as epistaxis, are most commonly caused by dry air. Nosebleeds occur when the blood vessels that line the inside of your nose break and bleed. Therefore, it’s important to keep the inside of your nose moist. Here are 5 helpful tips to prevent nosebleeds during this holiday season!
- Humidifier: Purchase a small humidifier to moisturize the air and your nasal membranes while you sleep. You can also use it during the day. Be sure to clean it regularly so mold and bacteria doesn’t grow.
- Saline nasal spray: Spray 2-3 squirts of saline spray in each nostril multiple times per day to keep the nasal mucosa moist. Examples of brands include Ocean™, Deep Sea™.
- Don’t pick your nose: Any picking or scratching of the nose can cause irritation to the mucosa and rupture a blood vessel, leading to a nosebleed. It could be helpful to trim your nails in case you accidentally scratch your nasal mucosa.
- Saline Gel: In addition to saline spray, nasal gels can also help keep your nasal mucosa moist. Examples of brands include Ayr™, Rhinase™
- Use nasal sprays correctly: Prescription nasal sprays can cause dryness when sprayed towards the septum (middle of the nose). This can increase your risk of nosebleeds. It’s important to use your right hand to spray in your left nostril and your left hand to spray in your right nostril.
Our office is always here to help! If you have any additional questions or concerns or if you are struggling to deal with nosebleeds this winter, call our office to schedule an appointment.
Practice Profiled in Suburban Life Magazine
Our practice was recently profiled in Suburban Life Magazine! Please click on the following link to see the article: montgomery-county-ent-institute-in-suburban-life-magazine
Additional Office Location
We are excited to announce that effective September 1st, 2016, the Montgomery ENT Institute will be merging with Dr. Sondra Saull’s office located in the Holy Redeemer Medical Office Building in Meadowbrook, PA. This union of teams will ensure the level of excellence in patient care that you have come to trust from both practices.
Both Dr. Schwartz and Dr. Ondik will continue to have hours at their Elkins Park office, but will now have additional hours at the new Holy Redeemer office. Dr. Saull will continue to see patients at the Holy Redeemer office.
Dr. Saull has been in practice for 30 years and is board certified in Otolaryngology, Head & Neck Surgery. She uses an integrative approach to the medical management of Ear, Nose and Throat conditions, and has a special interest in working with the older patient.
Dr. Schwartz founded the Montgomery County ENT Institute in 2007 to address a need for personalized and specialized care. With 20 years of experience, her passion for patient care has served patients of all ages in the Philadelphia region. She is board certified in Otolaryngology, Head & Neck Surgery and is a Fellow of the American Academy of Otolaryngic Allergy.
Dr. Ondik joined Montgomery County ENT Institute in 2014, and in addition to ENT care, is a double-board certified surgeon with a special interest in facial plastic and cosmetic surgery. He is board certified in Otolaryngology, Head & Neck Surgery and Facial Plastic and Reconstructive Surgery.
We look forward to continuing to serve our patients as the Montgomery County ENT Institute.
Sincerely,
Melissa Neumann Schwartz, DO FAOCO FAAOA
Sondra C. Saull, MD
Michael P. Ondik, MD
Montco ENT Partners with TrueHearing
Good news! Montgomery County ENT Institute has partnered with TruHearing to provide low cost, quality hearing solutions for individuals struggling with hearing loss, but were unable to afford help. Retirees and members of many union plans now have access to these new programs. If you have found the cost of obtaining new hearing aids beyond your reach, or if you want to experience the benefit of new technology available in hearing aids today, give use a call at 215 887 7380 today. We can schedule an appointment for you, and help you determine if you qualify for these exceptional programs.
When To Worry About A Sore Throat
Sore throat
A sore throat is a fairly common complaint, and there are many causes from post-nasal drip to more serious causes, like infection or tumor. Otolaryngologists are doctors who specialize in ear, nose and throat disorders. They are able to conduct a thorough examination with special scopes to visualize the throat and voice box, and evaluate the cause of your sore throat.
Could it be from allergies? Or a cold?
Post-nasal drip is when excessive mucus produced in the nose drains down the throat causing irritation. Allergies or an upper respiratory infection like the common cold can lead to post-nasal drip. A post-nasal drip from allergies can be seasonal or year-round. Allergy testing is beneficial to help identify which allergens are triggering your symptoms. Topical nasal steroid sprays and/or antihistamines can be helpful. If your symptoms persist even on medications, you may benefit from allergy therapy with allergy shots, allergy drops placed under the tongue or allergy tablets.
Could there be an infection causing my sore throat?
An infection of the tonsils, known as tonsillitis, is a common cause of a sore throat which is usually severe in intensity. It comes on quickly and is often accompanied by fever, pain when swallowing and swollen lymph nodes in the neck. Pus is usually present on the tonsils when it is bacterial. ‘Strep throat’ refers to the name of the bacteria (Streptococcus) that causes a common bacterial tonsillitis. This kind of throat infection should be treated with antibiotics; however a viral infection of the tonsils does not require antibiotic therapy. Both types of infections usually resolve within 7-10 days. A tonsillectomy may be necessary for patients who experience multiple episodes of tonsillitis each year.
Could it be related to my diet?
Acid reflux, also known as Gastroesophageal Reflux (GER) or Laryngopharyngeal Reflux (LPR), can cause recurrent sore throats. This is when acid from the stomach travels up into the esophagus and around the voice box causing inflammation. Many notice the sore throat is worse in the morning just after waking up, and this is due to acid reflux occurring during the night while you are sleeping. Heartburn and indigestion are not always present with LPR, and this is known as ‘silent reflux.’ Other symptoms include a dry cough, a sensation of mucus in the throat, throat clearing, hoarseness, and difficulty swallowing. Antacid therapy, such as Tums, Pepcid, Prilosec (Omeprazole) are a few of the over-the-counter medications that can help alleviate the sore throat caused by reflux when taken over a few weeks. It is important to treat acid reflux because it is a risk factor for cancer of the esophagus. Lifestyle changes are also important to help eliminate this problem causing your sore throat. Caffeine, chocolate, alcohol, spicy food, peppermints, acidic fruit juices are common food triggers of acid reflux. It helps to elevate the head of the bed when sleeping and to avoid eating late at night. A pH probe is a useful test to help diagnose and determine the severity of acid reflux. It entails having a small, thin probe placed into the nose and throat which can detect if acid is reaching the back of your throat. You can still eat, drink, and sleep normally while having the pH probe in place. This is a useful test since many patients have acid reflux at night when they are sleeping so they are unaware it is occurring.
Is this a symptom of something more worrisome?
Sometimes a sore throat is from a malignancy, or tumor, in the head and neck. If you have a sore throat that persists longer than 1-2 weeks, you should schedule an appointment with a medical provider. Certain symptoms, such as difficulty swallowing, a change in your voice, unexplained weight loss, or a lump in the neck raise a red flag of something more worrisome causing your sore throat, and you should see a medical provider immediately.
Turn Down The Volume
All About Allergies
What are allergies?
Allergies occur when your body’s immune system overreacts to substances that either enter or come into contact with your body. The word allergy covers many topics, but when people are complaining about “allergies” they are probably talking about environmental allergies. Environmental allergies include substances like dust, dander and pollen. These substances cause irritation of the nose and eyes and create symptoms like post-nasal drip, nasal congestion, itchy or watery eyes, sneezing, wheezing, and coughing.
How do I know if I have allergies?
You may already suspect that you have allergies, but your doctor will need to ask questions about your symptoms and your exposures in order to help determine if you are truly allergic. Some people suffer from seasonal allergies and notice that they have a runny or stuffy nose at certain times of the year or after they have been exposed to a cat or dog. Other people may have year-around symptoms without any seasonal variation and many patients will have both types of allergy. After your physician discusses your symptoms and exposures they will usually perform an allergy test.
How is allergy testing done?
Allergy testing is usually done in one of two ways. Typically, your physician will order a “skin-prick” test that checks your body’s reactions to multiple allergic materials such as different pollens, cat dander, dust, etc. The test is well-tolerated by patients and takes about 45 minutes to do in the office. Alternatively, your physician may order a blood test. You doctor will help determine which type of test is best for you.
I was tested for allergies when I was a kid and told I wasn’t allergic.
Just because you may have been tested and shown not to have any allergies as a child doesn’t mean that you can’t develop allergies as an adult. Many patients develop allergies later in life.
What are food allergies?
Food allergies occur when your body reacts to any food such as peanuts, shellfish, milk or eggs. You may experience symptoms such as tingling or itching of the mouth, hives, nausea, wheezing, or even more severe reactions such as anaphylaxis.
There is also a condition called “Oral Allergy Syndrome” where patients with pollen allergies also have reactions to specific related foods. For example, someone with a ragweed allergy may have a reaction to bananas or melons. Symptoms are usually limited to an itchy mouth or throat but they could be more serious.
What do allergies have to do with asthma?
Both allergy and asthma are the result of your body’s overreaction to exposures in the environment. A typical allergy patient reacts by experiencing nasal and/or eye symptoms. An asthma patient reacts with wheezing, cough or difficulty breathing. Many patients will have both conditions to a greater or lesser degree. It is estimated that 70-90% of patients with asthma have nasal allergies and 40-50% of patients with nasal allergies have asthma. Uncontrolled allergies may worsen asthma symptoms. In fact, many asthma patients find that their breathing problems are better controlled when their allergy symptoms are treated. We treat both allergy and asthma together at our practice.
What treatments are available for allergies?
There are three main treatments for allergies. The first treatment is avoidance, and as you would expect, it means trying to keep away from the substances that produce an allergic reaction. Avoidance measures include removing carpets and upholstery (to eliminate dust mites), keeping your windows shut in the warm months, using air filters, and protective covers. The second type of treatment includes the use of special medications such as nasal sprays, oral antihistamines and other medications. The third line of treatment is immunotherapy. Immunotherapy (also known as “allergy shots”) is a technique where your doctor uses small doses of allergic material to help your body learn not to overreact. At our office we offer the traditional allergy shots as well as a newer technique called allergy drops. Allergy drops have the advantage of allowing you to administer the therapy yourself at home without the need for any injection.
Can allergies cause sinus and ear infections?
Allergies have the potential to lead to many other issues including sinus and ear problems. Your sinuses are connected to your nasal passage through very small openings. Allergies cause these openings to swell, leading to a build up of mucus and infection within the sinuses. Similarly, allergies can cause swelling and blockage of the eustachian tube that connects the nasal passage to the part of the ear. Blockage of this tube can lead to a feeling of pressure in the ear, a build up of fluid, or a middle ear infection.
What can I do if I suspect I have allergies?
The best course of action is to meet with one of our physicians or our physician assistant to have a detailed discussion about your symptoms followed by a thorough examination with possible allergy testing.
Is My Sore Throat From Acid Reflux: Understanding LPR
What is laryngopharyngeal reflux, or LPR?
This is a common disorder where acidic contents from the stomach go up beyond the esophagus and into the area around your voice box creating irritation and inflammation. Small amounts of acid can damage this area of your throat since it is not equipped like the esophagus to handle acid exposure. As few as 3 reflux episodes can cause severe laryngeal inflammation and injury.
What is “silent reflux”?
This is the name given to LPR since many patients do not experience classic heartburn or indigestion, and in fact, may be completely unaware it is occurring. Some common symptoms of LPR include hoarseness, a feeling of mucus in the throat, or throat clearing. It may occur when you are upright or lying down.
How is LPR diagnosed?
Swelling and irritation around the voice box can be indicative of acid reflux. Your ENT provider has special scopes to visualize this area in the office.
A 24 hour pH probe monitor is a great test to objectively measure and confirm acid reflux. This test detects acid that occurs above your esophagus. A small probe is placed into one nostril and sits above the back of the throat. It does not interfere with eating, drinking or sleeping. This test is more sensitive in diagnosing LPR than traditional pH testing. Additionally, this test is easy to administer, is more comfortable and less expensive than standard pH manometry.
What is the best treatment for LPR?
Your doctor may prescribe a Proton-Pump Inhibitor (PPI) or a different class of antacid medication. It is important to take the medication every day as prescribed. It can take 4-6 weeks for the inflammation to appear improved on exam.
Besides medication, lifestyle changes are very important. Elevation of the head of the bed (using wooden blocks or a wedge pillow) is a great way to decrease acid reflux at night. Some studies show this to be more effective than medication. Avoidance of caffeine, chocolate, acidic juices (OJ, Grapefruit), peppermints, and spicy food help. It is beneficial to stop eating 2-3 hours before lying down, and to eat smaller, more frequent meals rather than large meals.
Why is it important to treat LPR?
Laryngopharyngeal reflux has serious potential consequences. Barrett’s esophagus is a precancerous condition of the esophagus that happens in a small percentage of people who have acid reflux. Chronic acid exposure creates changes in the esophagus which can potentially become cancer of the esophagus. It is important to have routine checkups with your ENT provider.
Understanding Your Allergies and Sinuses
Please join Dr. Michael Ondik on May 20th at 7pm for a patient seminar at the MossRehab Einstein Elkins Park at 60 Township Line Road, Elkins Park, PA 19027. The seminar will discuss treatment of allergies and sinus disease and offers patients an opportunity to learn more about their condition. The seminar will be in the G1 Conference Room. Please call our office at 215-887-7380 with any additional questions about the upcoming seminar.
Dealing with Facial Skin Cancer
Dealing with a skin cancer can be a very stressful experience. When the cancer is on the face, it may pose serious functional and cosmetic issues. Facial skin cancers can be removed and repaired by a Facial Plastic Surgeon. Sometimes the cancer may be removed with a procedure called Mohs Surgery, performed by a specially trained Dermatologist called a Mohs Surgeon. Repairing the resulting defect may require a Facial Plastic Surgeon.
Dr. Ondik is a Board Certified Facial Plastic Surgeon and has extensive experience in repairing all areas of the face, including total nasal reconstruction. Dr. Ondik will coordinate with your Dermatologist or Mohs Surgeon to remove and/or repair the resulting skin cancer defect. He will spend time explaining the repair options. Each skin cancer repair is carefully chosen to restore the function of the facial component and ensure the most cosmetically superior result.
New York Times report on Hearing Research
In recent months there has been some exciting developments in hearing research. The New York Times recently reported that pharmaceutical companies have turned their attention to helping people with ear disorders. Hearing loss, tinnitus and dizziness occur when there is significant damage to structures inside the ear, called hair cells. They are using gene therapy to help regenerate areas of the cochlea where hair cells have been damaged. Some companies are having small successes, others, not so much. The good news is that they seem to be on the right track and we are monitoring their every discovery. Take a look at the article. Let me know if you found it as fascinating as I did.
New Treatment for Nasal Polyps – PolypVac on “The Doctors”
New Allergy Tablets for Grass and Ragweed Sufferers
An effective way to treat seasonal grass or ragweed allergy. This is a convenient option for patients who are not able to commit to weekly allergy shots, patients who have a needle phobia, or patients who suffer from seasonal allergies due to grass or ragweed. A rapidly dissolving tablet is placed under the tongue every day in order to reduce allergic symptoms. Therapy should start around January for grass, and May for ragweed, and should be continued throughout the season. The first tablet is given in the office and the patient is observed for 30 minutes. A prescription is given for the grass tablets to be taken at home. Grastek is approved to treat children 5 years and older; Oralair is approved for ages 10-65 years old; Ragwitek is approved for adults 18-65 years old.
BPPV, a Common Cause of Dizziness
There are many causes of dizziness, but one particular cause can be easily treated. Read more about a common type of dizziness called BPPV:
Liquid Rhinoplasty
While there has been an explosion of injectable fillers being used for facial lines and wrinkles, many patients are not aware that these same fillers can be used to improve the shape of the nose. The procedure is called “liquid rhinoplasty” and uses injectable fillers to smooth out depressions or hollows. In some cases the filler can also be used to help camouflage small bumps or humps on the nose. The procedure isn’t permanent, but the results may last up to a year or slightly more. It may be perfect for the patient that has a small nasal imperfection that isn’t interested in surgery.
